Intelligent Revenue Management™ for European Healthcare. Apylon helps providers increase revenue, reduce costs and streamline billing operations.
How we help our customers
We make healthcare billing accurate, compliant, and scalable
Providing healthcare is complex - getting paid shouldn't be.
Demand for healthcare is exploding and the catalog of treatments is evolving exponentially - payers enforce stricter rules and more rigorous claims reviews while billing workflows remain manual and error-prone. Apylon evens the scales.
Meet your AI powered Revenue Management Engine
We build your engine. Through applied machine learning on historical claims data and rule-based algorithms grounded in industry knowledge, Apylon creates your proprietary Revenue Management Engine.
- Deterministic rules available to AI agents and humans
- Auditable decision making — no black box
- Single source of truth for payer contract interpretation
- Continuously learning and self-improving
Products
Apylon works across the billing life-cycle with a mix of hosted applications, autonomous AI agents and integrated co-pilots.

Revenue Analysis. We do an initial intake to identify revenue opportunities and automation potential based on your claims data.

Billing Agent. Automates claims using payer rules, coding guidelines, and historical outcomes to ensure accurate submission.

Billing Co-pilot. Supports medical billers with real-time guidance and validations for accurately handling complex claims.

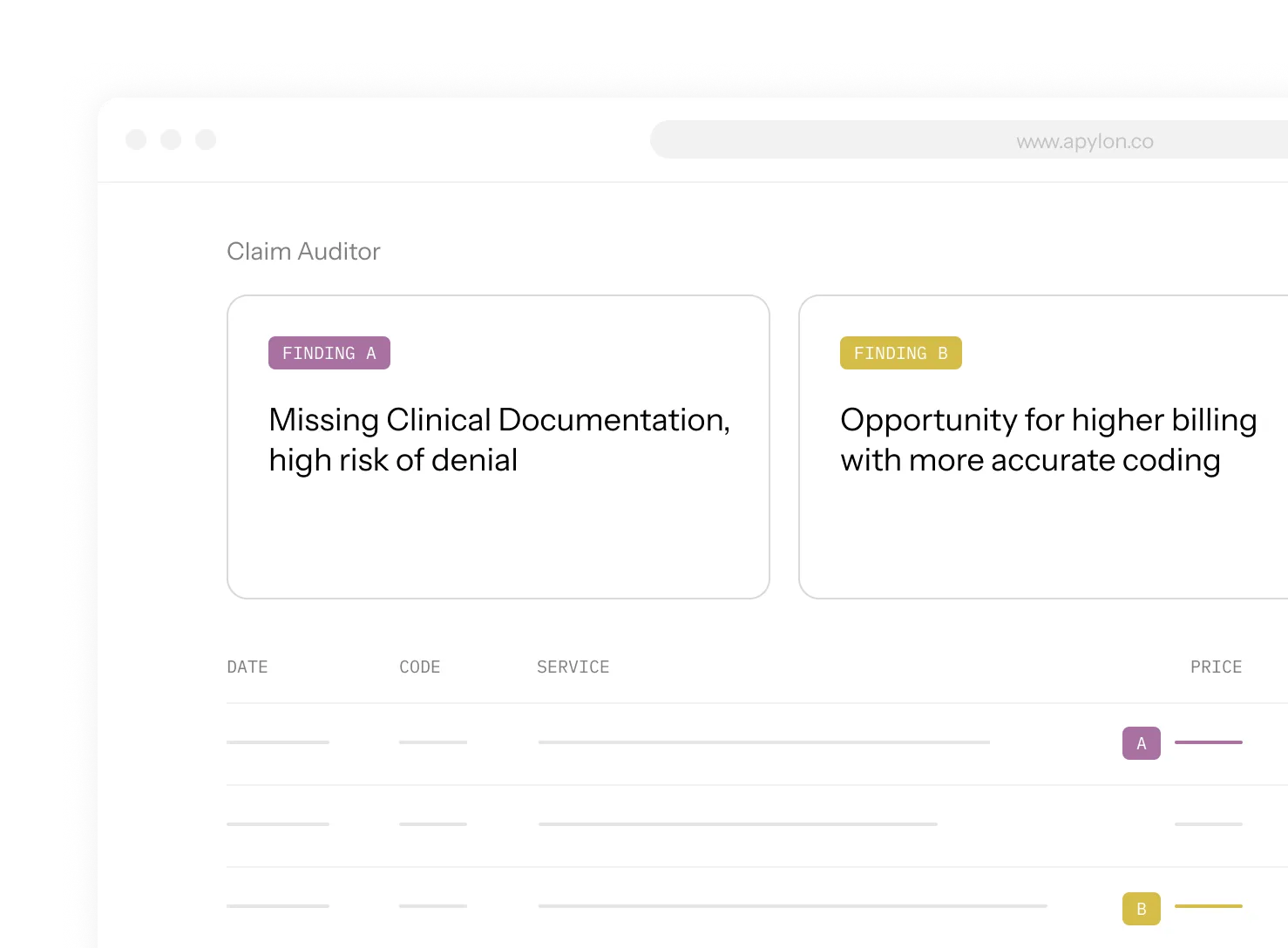
Claim Auditor. Reviews claims against payer and coding rules to detect errors, missed charges, and compliance risks.

Clinical Documentation Integrity. Identifies documentation gaps that affect coding accuracy and reimbursement.

Denial Mitigation. Reduce denial rates by spotting risks up front and automatically create comprehensive appeals.
Platform
Get started in weeks, not months with our turn-key platform. When you're ready, integrate it into your existing workflows and systems for minimal change management.
{
"audit_id": "84a849c41",
"status": "completed",
"findings": [{
"type": "billing_risk",
"severity": "high",
"confidence": 0.92
}],
"billing": {
"amount": 1240.00,
"currency": "EUR"
}
}Cases
Proven results from EU based hospitals
Real world results from our forward thinking hospital and clinic partners.
By building and employing their own revenue compliance engine, our partners have seen materially improved billing accuracy and financials at scale.